Food, Global Health Reading time 4 min
Understanding and managing epidemics in livestock
Published on 30 April 2020

How can we effectively anticipate epidemics?
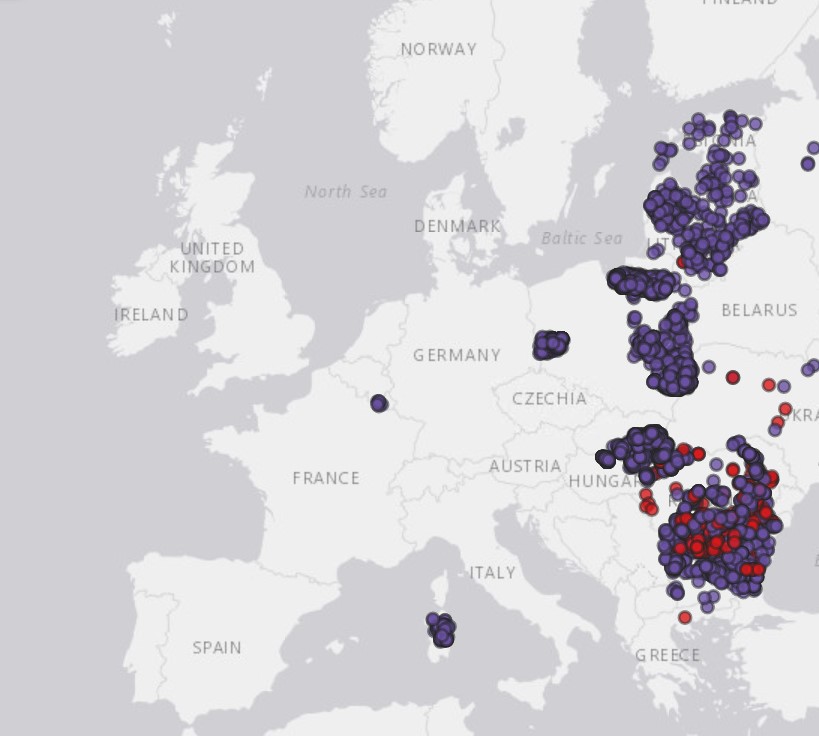
Christian Ducrot: For known diseases, monitoring programmes are already in place at national, European, and global scales. The French platform ESA tracks the risk of around 20 diseases that occur in livestock and wild animals in France. INRAE has contributed to ESA since 2018 (1). At the international level, there is also continuous monitoring of highly pathogenic avian influenzas (HPAIs) (2), African swine fever (ASF), and bluetongue disease. Interactive maps show outbreaks in different countries and their temporal dynamics (3). This surveillance system was crucial in helping France rapidly detect the sudden arrival of Schmallenberg virus in 2012 as well as the outbreaks of bluetongue disease in 2006 and 2015.
There are also diseases that are under control but that must be monitored because they remain endemic. For example, in 2001, France was officially declared free of bovine tuberculosis (bTB) (4) by the European Union (5), but there have been recurrent outbreaks of the disease since 2004 in certain regions of the country, notably in Dordogne. Several types of wild animals, such as foxes, deer, boar, and badgers, can act as reservoirs for the bacterium causing bTB. It is for this reason that the pathogen's presence is monitored not only on livestock farms and in slaughterhouses, but also in zones where livestock and wild species may interact, such as watering holes or grazing sites. In this way, high-risk rangelands can be better managed.
The utility of ESA goes beyond helping to detect when epidemics are headed towards France. The platform can also be used to coordinate surveillance and health protection efforts within the country.
Additionally, it is important to establish research strategies that anticipate future health crises. Researchers need time to prepare. Such is the role of the RFSA network, which allows stakeholders focused on animal health to coordinate their efforts (6). The network prioritises actions that promote research, drug development, testing, and vaccines. For example, RFSA manages publicly funded grant programmes for bluetongue disease research.
Once an epidemic has occurred, what is the next step?
C. D. : If we have enough information about the pathogen causing the disease (e.g., its hosts, mode of transmission, virulence), we can build models. At INRAE, we have amassed substantial modelling expertise, and we have developed several types of powerful modelling approaches to use in different contexts.
What is the purpose of these models? To start off with, they allow us to explore different sets of circumstances to better understand and manage epidemics. For example, INRAE researchers have developed a model that has helped manage bovine paratuberculosis (7). First, the model underscored the importance of verifying the health status of animals introduced into a herd—it found that, 40% of the time, the presence of just one infected animal could result in the herd remaining persistently infected over a 20-year period. Second, the model found that calves primarily become infected after being contaminated by faecal matter from adults. Other modes of transmission (e.g., in utero or via milk) appear to be less important. Consequently, strategies for managing bovine paratuberculosis should focus on verifying the infection status of new animals and having dedicated pastures for calves. For each disease, modelling can identify the key factors that we should target when designing effective control strategies.
Models can also teach us a great deal about epidemics a posteriori. For example, for bovine spongiform encephalopathy (BSE), modelling allowed us to reconstruct infection periods and to estimate the value of R0 over time (R0 is the mean number of new infections resulting from a single previous infection). We were also able to understand how some animals ended up with BSE even though they were born after the ban on feeding cattle with meat-and-bone meal (MBM), the practice responsible for the spread of the disease (8). These animals are referred to as BARBs (born after the imposition of the reinforced feed ban). We had several hypotheses. For example, we thought that calves could become infected in utero or via the ingestion of dietary fats coming from infected animals. In fact, there was an entirely different explanation: the animals had become infected because their diets contained swine or poultry feed, which included trace amounts of MBM. It was the correlation between the number of BARBs and local densities of swine and poultry that led to this discovery, which was then confirmed by specifically studying the diets of these BARBs over the course of their lifetimes.
How can we reduce the risk of epidemics in livestock?
C. D. : One major factor causing epidemics is high animal density. In addition, in farming systems in Southeast Asia and China, there is contact among different species, such as swine and poultry, and livestock live in close proximity to humans. When species swap viruses, genome rearrangements can occur, leading to the emergence of pathogens that pose a threat to human health. When epidemics occur, they can cause major harm to both large and small livestock farms. We carried out an a posteriori study on the H5N1 avian influenza epidemic in Thailand, which affected about 1,700 family farms and caused 25 flu cases in humans. Although it was thought that the disease persisted locally because of migratory birds or fighting roosters, our research showed that disease dynamics were mediated by poultry collectors, who travel from farm to farm as they gather animals for transport to the nearby slaughterhouse. In this case, commercial farms were less hard hit than family farms because the former were able to impose draconian quarantine measures and they had well-structured systems for transporting poultry to slaughterhouses. They were thus able to limit disease transmission and continue exporting their products. Our work helped veterinary services in Thailand develop new programmes to control the transmission of H5N1 by targeting the actions of various key stakeholders.
As the H5N1 epidemic also illustrates, the movement of animals plays a key role in the spread of epidemics. Health risks climb as livestock farming becomes more intensive: the segmentation of production systems leads to massive animal transfers. For example, calves may be reared in France but fattened in Italy, and, for poultry, egg production is entirely distinct from chick rearing.
Once the major factors driving epidemics have been identified, what are the next steps? First, it is important to act preventively. Livestock farmers should receive training in biosecurity measures such as quarantining newly acquired animals, placing double rows of fencing between grasslands, ensuring visitors respect health and safety guidelines, and disinfecting buildings and fertiliser spreaders. Vaccinating livestock is also an effective preventive measure, if a vaccine is available. Furthermore, it is also crucial to monitor outbreaks in real time to contain them quickly; for example, rapid action can be taken to limit the transfer of animals. Collecting reliable epidemiological information early on is essential when implementing effective health measures.
- Read the article (in French)
- All currently known types of highly pathogenic avian influenzas (HPAIs) are H5 and H7 subtypes.
- International health surveillance efforts are led by CIRAD and ANSES.
- Bovine tuberculosis also poses a health threat to humans; it is responsible for fewer than 1% of tuberculosis cases in France, but this figure climbs to 10% in certain countries (source: World Organisation for Animal Health). While it is difficult to diagnose, it affects livestock on around 100 farms per year in France. It is one of the diseases for which France funds a permanent surveillance and control programme.
- Over the last six years, bovine tuberculosis has affected fewer than 0.1% of herds.
- The French network for animal health (RFSA) is composed of ANSES; the French Ministry of Higher Education, Research, and Innovation; various research institutes; French veterinary schools; and the French union of pharmaceutical companies (LEEM), among others.
- Bovine paratuberculosis is among the infectious diseases with the greatest economic impact in dairy cows. Calves of up to one year of age are highly susceptible to infection, which can occur via different pathways: in utero, through the milk, and/or via the presence of contaminated faeces in food. Symptoms may take up to 15 years to appear.
- In France, hundreds of animals born after the ban on MBM (in 1990) have been afflicted with BSE.
It is important to define and limit agricultural intensification. Intensive agriculture aims to enhance production by increasing the quantity of meat, milk, or eggs produced per animal, hectare, or hour of work. The main techniques for intensifying production on livestock farms involve breeding animals based on their genetics, modifying diet composition, increasing animal density, and incorporating automation. When breeding programmes are overly focused on enhancing traits related to production, other traits are left by the wayside, notably robustness and disease resistance. Consequently, animals can become more vulnerable to infections in general. Because livestock are more susceptible to disease and are living under higher-density conditions, the use of antibiotics is greater. Resistant bacteria emerge as a result (1), an outcome with major consequences for human health.
As the repercussions of agricultural intensification have become clear over the last several years, a movement against this form of farming has swelled within the general public. At INRAE, we are developing agroecological approaches to crop and livestock farming that promote ecosystem equilibrium (2). Furthermore, in 2012, France launched a national programme to promote the responsible use of antibiotics, which has led to a decline of more than 30% in antibiotic usage on French farms.
(1) This phenomenon is the result of the excessive use of antibiotics both within livestock populations and human populations.
(2) On livestock farms, these approaches include broadening the suite of criteria used in animal breeding; giving ruminant livestock greater access to grasslands; better incorporating co-products from local crops into swine and poultry feed; promoting mixed crop-livestock systems; and enhancing protein self-sufficiency on livestock farms to limit reliance on imported sources
