Food, Global Health Reading time 4 min
Promising anticancer research using protozoa
Published on 12 November 2020
Most antitumour treatments—known as conventional treatments—rely on surgery, radiotherapy, and chemotherapy. Many types of cancer respond poorly to these treatments, which have multiple side effects. Immunotherapy is a new and promising approach that consists of educating the patient’s immune system to effectively fight cancer cells. Numerous possibilities are being explored, in particular using living microorganisms, which are able to stimulate the immune system but also to invade and destroy cancer cells. A research team from INRAE and the University of Tours, specialized in Apicomplexa protozoa, has presented a very promising lead by proving that protozoa can be used as an effective anti-cancer immunotherapy.
How does this anticancer immunotherapy work?
Isabelle Dimier-Poisson: The first thing we must understand is that tumour cells are constantly being formed in our bodies, and that, luckily for us, our immune system usually eliminates them... or, at least, up until the tumour being formed manages to inactivate these defence mechanisms. The idea behind immunotherapy is to reactivate these defences and one way of doing it is by introducing a foreign microorganism into the body, such as a virus, bacterium, or protozoan. This concept originated at the end of the 19th century, but it has only taken off in the last fifteen years or so, with the progress of molecular biology. The key is to really understand the microorganism being used in order to optimize its efficiency, while still guaranteeing its safety. A microorganism has different effects on the developing tumour. First, it invades the cancer cells, breaking them down. Then, the breaking down of the cells frees molecules which reactivate the immune system—suppressed by tumour cells. And, finally, the microorganism promotes the recruitment of immune cells to the site of the tumour. Additionally, it is possible to increase the efficacy of this microorganism by modifying it to secrete effectors that reinforce the stimulation of the immune system (1), or therapeutic antibodies that contribute to reverse the immunosuppression caused by the tumour cells (2). With their multiple possibilities of action, oncolytic microorganisms are the Swiss army knife of cancer therapy.
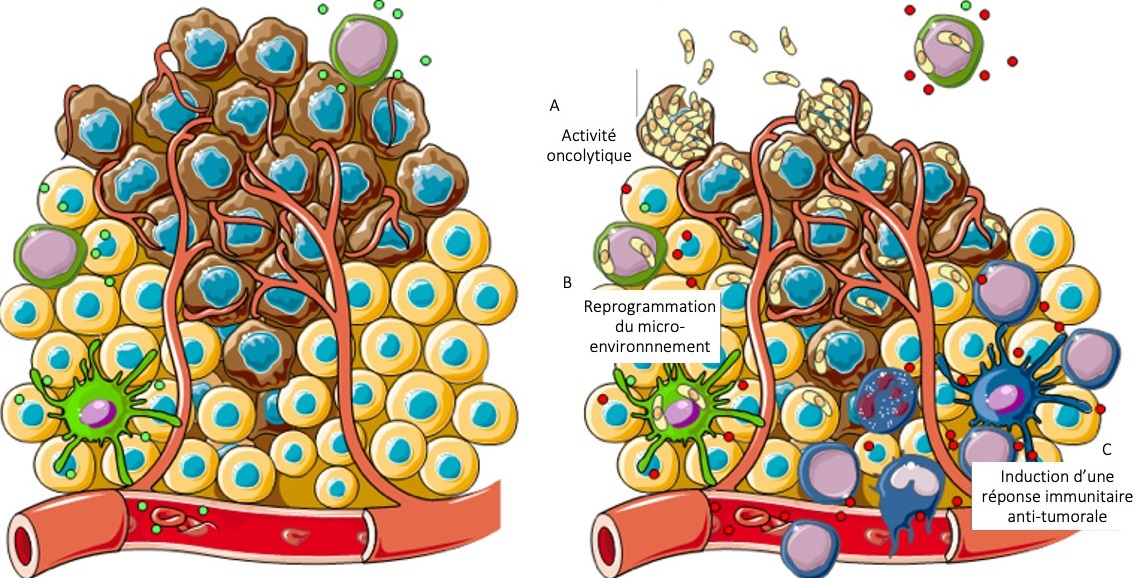
Treating tumours by means of microorganisms consists of three main mechanisms: (A) Breaking down tumour cells. (B) Reactivating the immune system, suppressed by tumour cells. (C) Recruiting immune cells to the site of the tumour.
What are the advantages of using Neospora caninum?
I. D-P: Neospora caninum is a protozoan infecting dogs as its definitive hosts and ruminants as intermediate hosts. It does not present any danger to human beings as it does not cause any illness. Unlike potentially dangerous oncolytic viruses of human origin, it can be used without the need to be inactivated or attenuated. Besides, protozoa are unicellular eukaryotic organisms with a fairly large genome, contrary to viruses. Their genome can easily accept additional genes, specifically genes that can help to fight cancer. This is what we did. We developed a protozoan strain able to secrete interleukin 15 (a powerful stimulant of the immune system) and antibodies capable of restoring the immune response suppressed by the tumour. We can also modify the protozoan to express an antibody specific of the cancer cell at its surface—so it only infects this kind of cells. We were able to prove that by injecting this “fully-armed” protozoan in mice carrying a human tumour (3), we could achieve, in just a few days, near-total regression of malignant tumours! Another advantage of the protozoan: it is completely eliminated from the body due to natural immunity but can be reused in the same patient without a loss of efficacy.
When will the treatment be available?
I. D-P: Our work has been the subject of two patents and one article in the Journal for ImmunoTherapy of Cancer. It has also led to the creation of a biotechnology company, Kymeris, which designs and develops anti-cancer immunotherapy products. We are currently working on the large-scale production of protozoa. We hope to start new clinical trials for patients with stage IV glioblastoma, as a result of our close collaboration with the neurosurgery department of the Regional University Hospital of Tours. We continue to work and our results are extremely promising in five models of poor prognosis cancer, those for which current therapies have proven unsatisfactory. Parallel to its use in human health, we hope that this protozoan could also be used in veterinary medicine, particularly to treat animals such as horses and pets—dogs, cats etc.
- Interleukin or interferon
- Tumour cells that bypass the immune system induce the appearance of receptors at the surface of immune cells (lymphocytes) that cause their depletion and inactivation. The antibodies used in this therapy bind to these receptors and restore the immune response.
- Merkel cell carcinoma, a rare but very aggressive cancer that mainly affects the elderly.
Reference: Lantier et al. 2020. Neospora caninum: a new class of relevant biopharmaceuticals in the therapeutic arsenal against cancer. Journal for ImmunoTherapy of Cancer, accepted for publication on 2 October 2020. doi:10.1136/jitc-2020-001242
Associate institutions: INRAE, University of Tours, University of Angers, INSERM, University Hospital of Tours and University Hospital of Angers.
Anticancer immunotherapy using viruses, bacteria, or protozoa has been explored for over a century. Two German doctors came up with the concept. From 1868 on, they observed an improvement in cancer patients that had contracted a bacterial skin infection. Since the 2000s, this method has been the subject of active research and increasingly sophisticated microorganisms are being used in clinical trials, sometimes as a complement to chemotherapy. Here are a few examples of "winning" cancer/microorganism associations:
- 1890: Sarcoma / Streptococcus pyogenes (skin infection)
- 1969: Lymphoblastic leukaemia / Bacille de Calmette-Guérin (BCG)
- 1976: Superficial bladder tumours / BCG
- 1970s: Mouse mammary tumours / Protozoan Toxoplasma gondii
- 2005: Head and neck cancers / Adenovirus H101
- 2015: Metastatic melanoma / Attenuated herpes virus expressing GM-CSF (immunostimulant)
- 2018: Canine Osteosarcoma / Attenuated Listeria monocytogenes bacterium
- 2018: Glioblastoma / Attenuated PVSRIPO virus
